Communicating the Radiation Treatment Experience
for the University of Chicago Comprehensive Cancer Center
Project brief
Currently, educational materials for patients undergoing radiation treatment are verbally dense and full of medical jargon. As a result, patients have difficulty understanding their upcoming course of radiation treatment, causing anxiety and uncertainty in an already stressful medical situation. In this project, we developed a visual communication tool that helps doctors inform cancer patients about radiation therapy and their specific treatment plan. The tool is intended to increase awareness around radiation therapy and decrease patient anxiety about treatment.
Co-project lead; project advised by Prof. Tomoko Ichikawa.
Additional team members: Laura Biltz, Apoorva Shenoy, Yanyan Li, Yachu Feng, Andrea Everman, Sarah Braunstein, Isabel Dec, Sonia Lala.
Current State of Patient Education
Patients are given resources at initial consultation and/or can look online. Resource materials are text heavy and written at an 11th-12th grade reading level. There are few relevant visuals, and the information is mostly general (i.e., not relevant to a patient's specific cancer site). Physicians and nurses supplement these resources with verbal review of treatment strategy during the initial consult appointment.
Research Planning
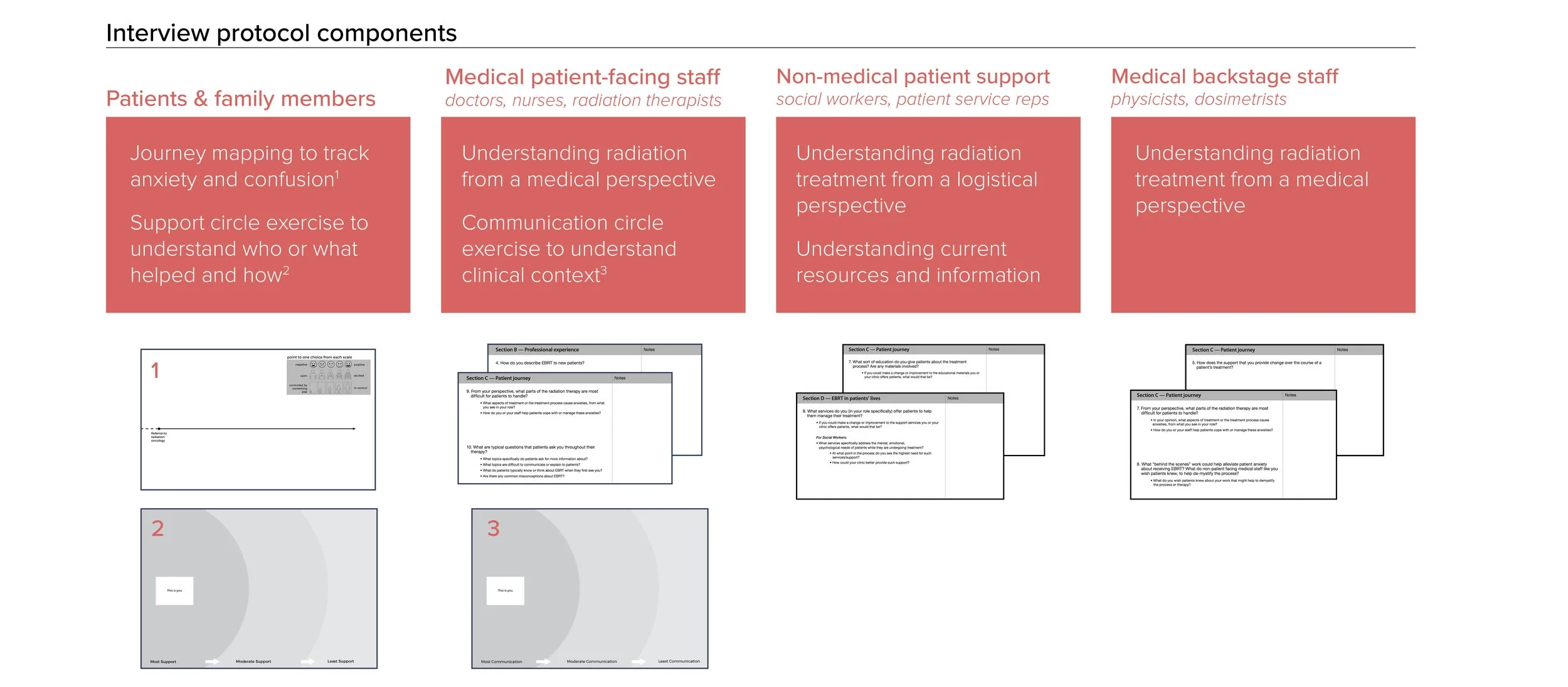
I co-led development of research protocols, which involved different interview guides for patients, medical providers, and patient support staff. Additionally, we developed activities to elicit richer information than might come out of traditional one-on-ones. This research addressed the following objectives:
• Understand radiation therapy & provider's role in treatment
• Understand in-clinic patient journey from consult to post-treatment
• Understand outside factors affecting patient journey
Research and Observations
We visited the University of Chicago radiation clinic for observations, and conducted 26 interviews in 2 weeks. In addition to conducting interviews and observations, I supported the team by adapting protocols after initial interviews to account for unforeseen topics and conversation flows.
Synthesis
After completing fieldwork, our first task was to distill the data from interviews and observations into content that could be used in a communication tool for patients. To do this, we categorized information by treatment phase (see columns below) and type of information (rows). This was the first step towards making our large volume of data useful.
Moving from insights to action
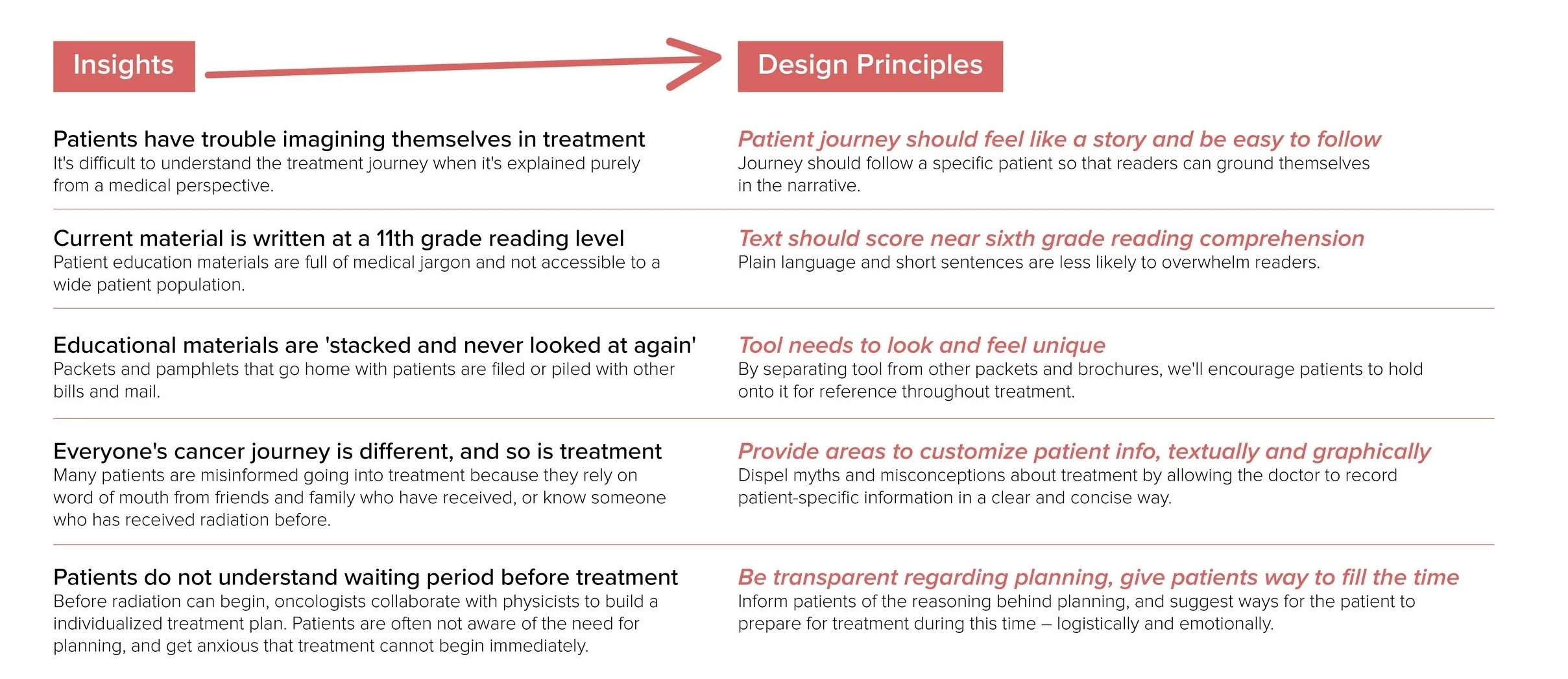
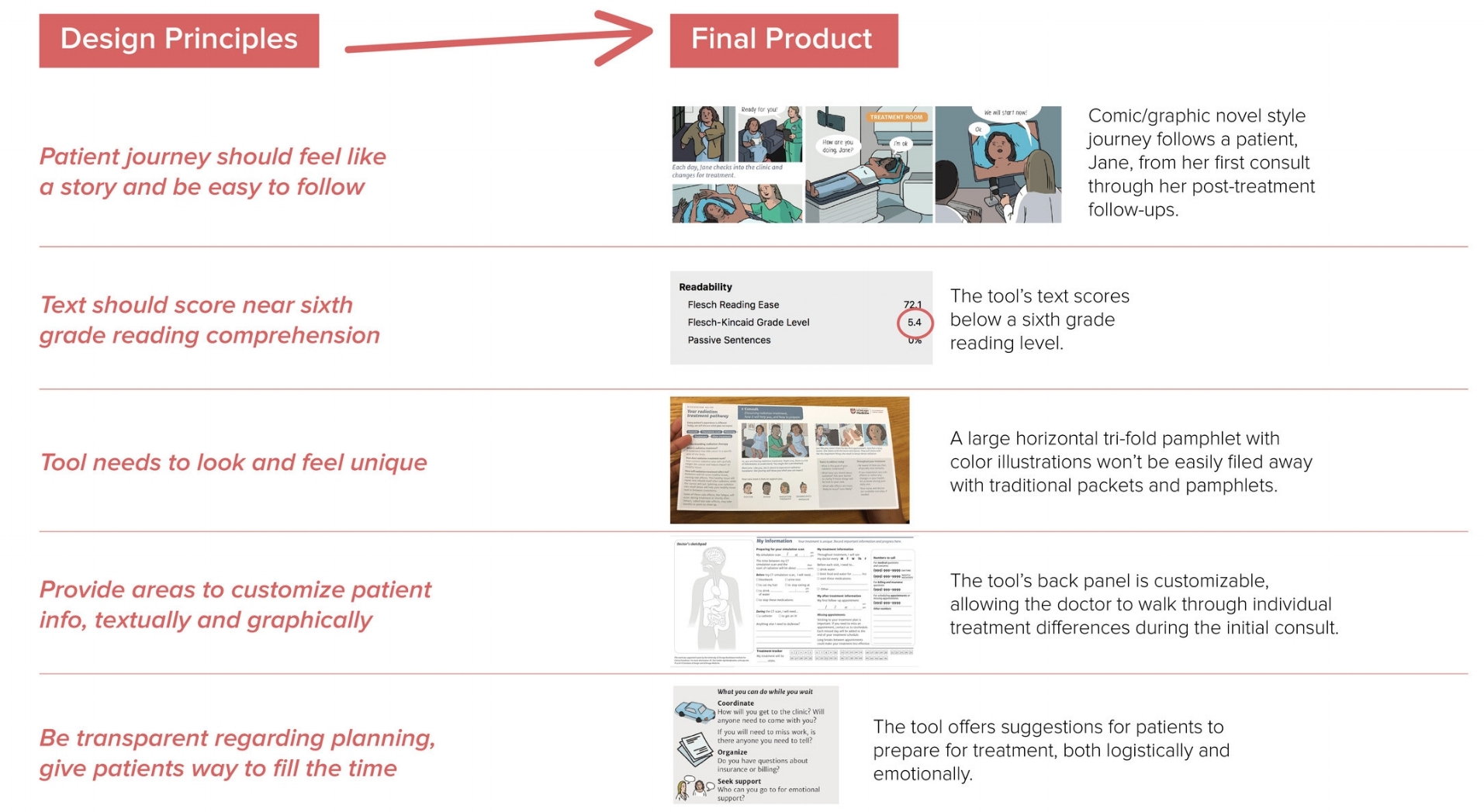
Next, we took a more macro perspective, integrating our primary research findings with secondary research on current patient materials. This allowed us to create insights
that directly drove the design of our communication tool. Here's a sampling of these insights and their resulting design principles.
Prototyping
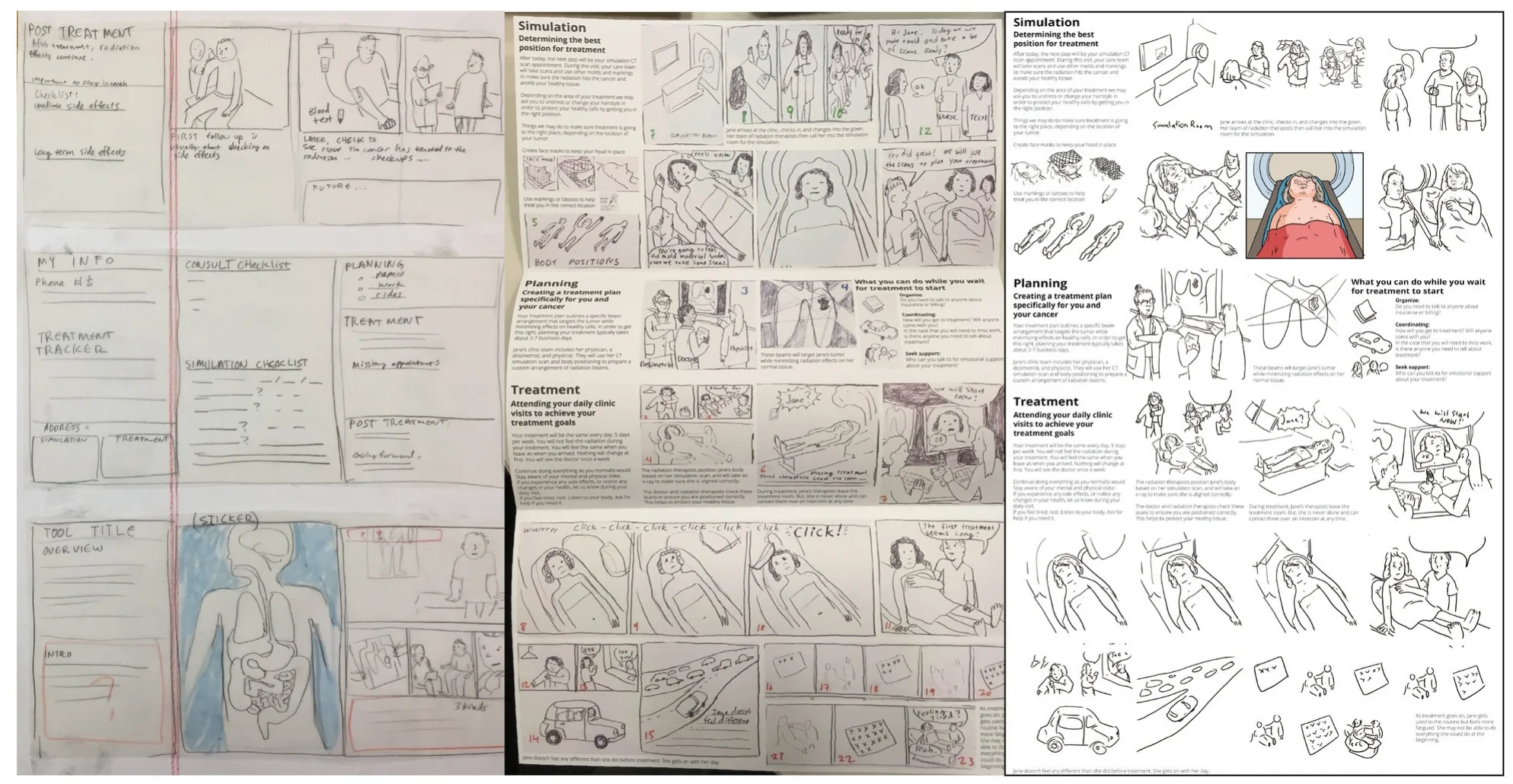
In prototyping we moved quickly from iteration to iteration, starting with a loose patient journey and each week tightening the content. We split into three "teams": content strategy, illustration, and form factor. I worked on content strategy and also liaised with the other teams, making sure the illustrations partnered well with the information, and that the form factor served our space needs for each section. We collaborated with a radiation oncologist during this phase, making sure we were accurately representing the radiation treatment journey.
The journey from low to high fidelity.
Final tool
Front panel of the folded tool, showing the first phase of the patient journey (consult).
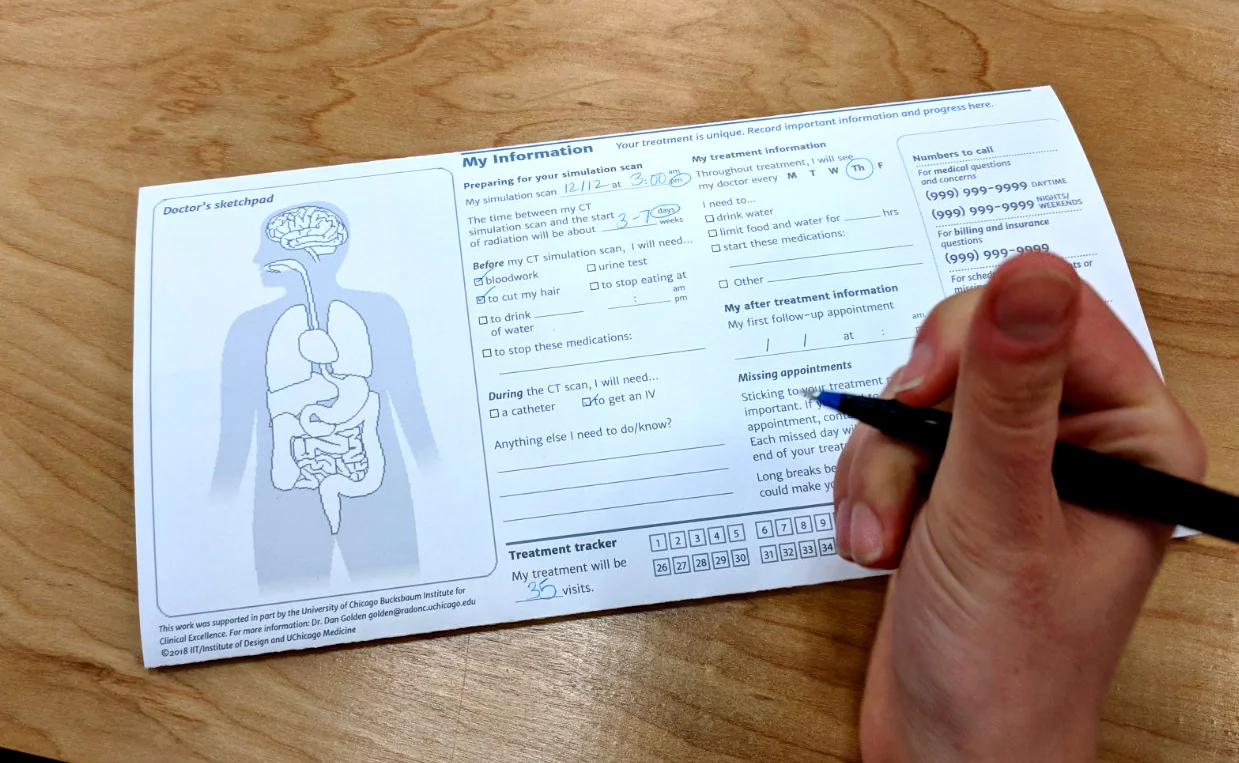
Back panel of tool includes a "My Information" section for doctors to personalize based on a patient's specific treatment plan.
Opened tool, showing the majority of the patient journey.
Final Presentation
We ended the project with a private presentation to UChicago physicians, representatives from the Bucksbaum Institute for Clinical Excellence (who funded the project), and Institute of Design faculty members with an interest in healthcare.